Eyelid Lacrimal and Orbit Anatomy
Our eyes are probably the most important vital structures we have in our body. They discovered on the surface by a thin layer of skin and soft tissue called the eyelids. The eyelids serve multiple purposes including protecting the eyeball from injury, controlling the amount of light that enters the eye and also constantly lubricating the eyeball with tears secreted by the lacrimal gland during blinking. All these functions together help maintain the structural integrity of the eyeball and protect them from external influences.
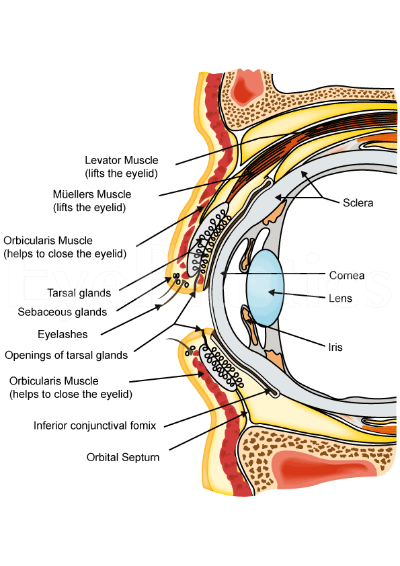
From an anatomical point of view, the eyelid consists primarily of skin, underlying soft tissue also called a subcutaneous tissue and a thin layer of muscle called the orbicularis oculi. Under this muscle are other issues that divide the area into different planes. These are called septum and include the fibrous orbital septum and tarsi. In adds to to this, in order for the eyelids to open are lid retractors that help assist blinking. Finally, there also exists a small amount of fat tissue as well. The eyeball is covered by a thin layer of tissue called the conjunctiva.
Anatomy of the eyelid
The description above only offers a superficial overview of the anatomy of the eyelid. If one were to look at the eyelid in a more detailed manner, a sagittal section taken across the eyelid will offer a clear view of the various structures that form it. Of course, it must be borne in mind that the structures that are visualised depend on the plane at which the sections are taken.
As mentioned above, the tissues can be divided into planes by structures called the septum. The orbital septum differentiates the orbital tissue from the lid. Behind the septum are a number of different other structures, a knowledge of which is essential if surgery is to be performed. In particular, it is essential to identify the anterior and posterior lamellae. In essence, the anterior lamella consists of the skin and the orbicularis oculi muscle while the posterior lamella consists of the conjunctiva and the tarsus.
Let's take a look at the structures of the eyelid in a bit more detail.
The eyelids
The upper eyelid starts at the eye and extends up words joined the skin of the forehead. It is distinguished from the forehead skin by the presence of eyebrows. Similarly, the lower eyelid starts at the eye and extends to join the skin of the cheek. Upon close inspection, it is evident that the Lord eyelid is a lot looser than the upper eyelid, particularly because the tissue within the cheek that blends with the lower eyelid is a lot denser.
At the top of the upper eyelid is a fold in the skin called a skin crease or the superior palpebral sulcus. It lies around 8 to 11 mm above the margin of the upper eyelid and consists of fibres of the levator aponeurosis. Similarly, there also exists another skin fold in the lower eyelid called the inferior palpebral sulcus. However, this skin fold is often more prominent in children and can become less prominent as one gets older. Anatomically, the inferior skin crease is seen around 3 to 5 mm below the outer aspect of the lid margin.
The inner aspect of the eyelid is called the inner canthal region. At this region runs a fold of skin called the nasojugal fold. From an anatomical point of view, this fold lies between the orbicularis oculi and the levator labii superioris. To put it in simpler terms, the nasojugal fold is that area of the inner aspect of the eye where tears roll down and can accumulate. It is also called the tear trough. Similar to the nasojugal fold is another fold of skin that is evident in the outer aspect of the eyeball. This is called the malar fold and runs from the outer aspect towards the nasojugal fold.
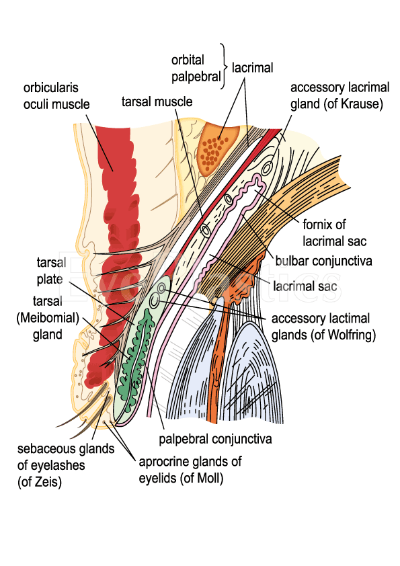
When the eyes are open, the space between the upper and lower eyelids is typically described as ‘fusiform’. This space is also called the palpebral fissure. Typically the palpebral fissure measures between 28 to 30 mm wide and around 9 to 10 mm in height. If one were to examine the palpebral fissure in a bit more detail, it would be evident that the highest point of the fissure lies at that point on the upper eyelid that corresponds to a point at the inner aspect of the pupil. Younger individuals have the upper eyelid slightly higher than older individuals in whom it lies at about 1.5 mm below the margin of the eyeball called the limbus. Similarly, the lower eyelid lies at the border of the lower limbus.
There are two points at which the upper and lower eyelids meet. The one on the inner aspect is called the medial canthus while that at the outer aspect is called the lateral canthus. Both of these have a unique angle at which the upper and lower eyelids meet. When examined along a horizontal plane, the medial canthal angle is located around 2 mm lower than the lateral canthal angle in Caucasians; it is 3 mm lower in Asians. The nose lies around 15 mm on the inside of the medial canthus.
In a nutshell, the palpebral fissure consists of the medial and lateral canthus, the lacrimal papillae (part of the tear glands, also called lacrimal glands) and a small opening of the lacrimal glands through the lower eyelid at the medial canthus called the punctum lacrimale.
Skin and subcutaneous tissue
The eyelid is primarily made of skin. It is the thinnest skin in the body and is less than 1 mm thick. Within the skin are a number of glands called sebaceous glands that secrete an oily substance called sebum. These glands are in larger numbers at the nasal aspect of the eyelid. If one were to trace back the skin of the upper and lower eyelid, it would be clearly evident that once it joins the forehead or the cheek, the texture of the skin changes and becomes a lot thicker. Furthermore, the texture of skin is also different at the various folds described above. Below the skin is a layer of thin connective tissue called a subcutaneous tissue (sub = under, cutaneous = skin).
.jpg)
Underneath the skin, along with the subcutaneous tissue is a thin layer of fat. However, the amount of fat is negligible when compared to other parts of the body. Typically, subcutaneous tissue is absent at points where the skin is attached directly to underlying ligaments such as the medial and lateral palpable ligaments. The skin and subcutaneous tissue can be subject to certain clinical conditions such as dermatochalasis and blepharochalasis.
Orbicularis oculi muscle
The orbicularis oculi muscle plays an important part in the function of the eyelids and also in facial expressions. When it contracts and relaxes, the skin over the muscle tends to move as well. The orbicularis oculi muscle is attached to the skin through fibres tissues that form what is called the superficial musculoaponeurotic system.
Broadly divided, the orbicularis oculi muscle consists of two main parts. The orbital part plays a role when the eyelids need to be tightly shut. It is further divided into pretarsal and preseptal segments. The other part is called the palpebral portion that plays a role in winking and blinking. The muscle is supplied by the facial nerve then divides into different branches to supply these different muscles. Anatomically, the facial nerve travels under the muscle groups and supplies it from under it surface.
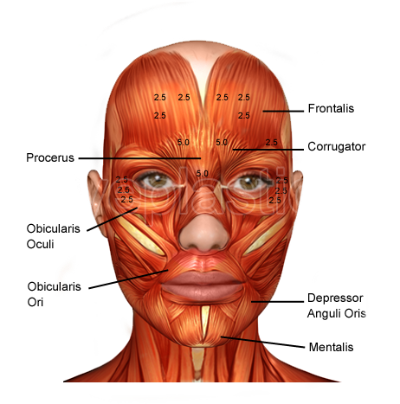
The orbital part of the orbicularis oculi muscle has a close relationship with other muscles responsible for facial expression. It originates from the inner margin of the orbit, further attaching to the upper and inner aspect of the orbital bone, the maxillary process that arises from the frontal bone, the lower and inner aspect of the orbital bone and the frontal aspect of the maxillary bone. The path taken by the muscle is typically described as 'horseshoe shaped'. The muscle fibres mingle with the surrounding facial muscles such as the corrugator supercilii and the frontalis muscle. As they travel around, they also interdigitate with the anterior temporalis fascia.
The preseptal portion of the orbicularis oculi muscle consists of a superficial and deep muscle head. The fibres of this portion that lie within the upper and lower eyelid join and the outer aspect to form a structure called the lateral palpebral raphe. The pretarsal portion also has similar origins and its fibres run under the lateral palpebral raphe, inserting into a bony structure at the outer aspect of the orbital bone called the lateral orbital tubercle through the lateral canthal tendon.
Submuscular areolar tissue
This is a loose connective tissue that lies beneath the orbicularis oculi muscle. It can form an anatomical plane that divide the eyelid into a front (anterior) and back (posterior) portion. The fibres of the levator aponeurosis then passed through this plane in the upper eyelid. A small portion of these fibres contribute towards the development of the upper eyelid crease. Similarly, in the lower eyelid, the fibres of the orbitomalar ligament passed through this plane.
If this anatomical plane were to be tracked towards the eyebrow area, the retro-orbicularis oculi fat will be traversed. If the plane were to be tracked towards the cheek, the sub-orbicularis oculi fat would be traversed.
Tarsi and Orbital septum
Tarsal plates
In order for the eyelids to maintain their shape and integrity, within them is dense fibrous tissue called tarsal plates. Each of these tarsi is around 1mm thick and 29 mm in length. There are 2 main types of tarsi – the superior tarsus and inferior tarsus. The superior tarsus is crescentic in shape and measures around 10mm vertically in its central aspect. It narrows outs as it traverses towards the nose and outer aspect of the eyelid. Its lower area is what forms the back of the eyelid that lies next to the conjunctiva of the eyeball. Similarly, the inferior tarsus lies in the lower eyelid, measures 3.5 – 5mm in height at its centre, and also lies in contact with the conjunctiva. Each of the tarsi are attached to the margin of the orbits through the medial and lateral palpebral ligament.
Within the tarsal plates are 25 tiny glands called mebomian glands. These glands are as tall as the tarsus, and they open at a point just in front of the lid margin where the conjunctiva meets the skin (mucocutaneous junction). If one were to look closely, they lie behind a grey line on the margin of the eyelid.
Medial palpebral ligament
Also called the medial canthal tendon (MCT), the medial palpebral ligament is a band of fibrous tissue that holds the inner aspect of the tarsal plates in place. It is closely related to the orbicularis oculi muscle and the tear ducts. The MCT is composed of an anterior limb which is formed by a small part of the superficial aspect of the orbicularis muscle that lies behind the tarsus. It traverses along a horizontal plane but is also attached to the frontal bone through a superior extension. The deeper part of the orbicularis muscle inserts into the back aspect of the lacrimal crest and the lacrimal sac fascia. The fascia of the lacrimal sac is therefore closely related to the various aspects of the MCT.
Lateral palpebral ligament
Also called the lateral canthal tendon (LCT), the lateral palpebral ligament is also a band of fibrous tissue that originates from the tarsus, traverses outwards under the orbital septum and eventually inserts into the lateral orbital tubercle (this lies around 1.5mm behind the lateral orbital rim). The LCT is around 10.5mm long and 6.5 mm wide, and at its midpoint attaches around 10mm below the frontozygomatic suture. The orbital septum and the LCT are separated by a pocket of fat called the Eisler pocket. In adds to, the LCT is attached to the outer part of the orbital rim through a superficial plane of fascia. This has been also called the superficial lateral canthal tendon and helps to keep the lateral canthus stable.
When traced above and below, the LCT attaches to the lateral horn of the levator aponeurosis above while the lower aspect forms an arc where it attaches. During outer movement of the eye (abduction), the lateral canthal angle moves around 2mm as well, and this occurs due to the fibres that attach from the back of the lateral check ligament of the lateral rectus muscle.
A structure called the lateral tarsal strap has been described by Flowers. This is believed to be different to the LCT, and connects the tarsal plate of the lower lid to the lower, outer aspect of the orbital rim. Anatomically, it is a broad and rather sturdy structure. It lies just 3mm below and 1 mm behind the LCT, and 4-5 mm behind the anterior orbital rim. If excised, it allows for elevation of the lateral canthus.
Orbital septum
A septum often refers to a band of tissue that separates a structure. The orbital septum is a connective tissue band that attaches to the border of the orbital bone at the periosteum (outer aspect of a bone). Within its central structure, the septum joins the lid retractors at the lid margins. If one were to look at the septum a lot more closely, it contains a number of layers (lamina) that are in close relationship with the anterior connective tissue framework. From a functional point of view, the septum has mobility similar to the eyelids.
We have already discussed how the septum attaches to the lid margin. If one were to trace the septum in an outward direction (laterally), it is evident that it is attached to the margin of the orbit, around 1.5mm in front of the attachment of the LCT. The orbital septum is separated from the LCT by the previously discussed Eisler’s pocket of fat. While traversing laterally, the septum runs along the rim of the orbit at the arcus marginalis. When traversing above and towards the nose, the septum runs across the supraorbital groove, in front of the trochlea and along the posterior aspect of the lacrimal crest. From an anatomical point of view, this position results in the septum lying in front of the medial check ligament and behind the lacrimal sac and Horner muscle.
When tracing the attachment of the septum, it passes the lacrimal sac fascia, eventually reaching the anterior lacrimal crest at a point corresponding to the lacrimal tubercle. It then passes below this crest and along the lower rim of the orbit, ultimately leaving the rim at a point beyond the zygomaticomaxillary suture. This results in creation of a small space (recess) due to its separation from the zygomatic bone - this is called the premarginal recess of Eisler, and is filled with fat. Eventually, the septum reaches the lateral orbital margin at a point that lies just below the Whitnall ligament.
Another extension of the septum exists from the point where the orbital septum joins the levator aponeurosis. Described by Reid et al, this extension travels over the tarsal plate and ultimately reaches the ciliary margin. The function of this septum is to aid the levator aponeurosis, and should be borne in mind when operating on the eye.
Orbicularis retaining ligament
Also called the orbital retaining septum or orbitomalar ligament, this ligament attaches the orbicularis oculi muscle to the lower rim of the orbit. It is weak in its central aspect, and a lot stronger in the lower-outer aspect. When traced laterally, it is contiguous with tissue that is formed by fusion of the outer part of the orbicularis oculi and the deeper periosteum and temporalis fascia. This fusion is called the orbital thickening. This orbital thickening covers the frontal process of the zygomatic bone.
As one gets older, the orbicularis retaining ligament tends to get thinned out and stretched, with these changes more prominent in the central aspect. When excised along with the orbital thickening, it results in full release of the superficial fascia that lines the orbital rim.
Upper lid retractors
The upper lid retractors are a group of muscles whose main function is the keep the upper eyelid elevated. The muscle that forms a part of this is called the levator palpebrae superioris (LPS). This muscle originates from the bottom aspect of the lesser wing of the sphenoid bone located within the skull. It consists of 2 heads - the levator muscle and the superior rectus muscle. They are joined together by fibrous tissue. From its origin, the LPS traverses horizontally forward for about 40mm, ending in an aponeurosis that is around 10mm posterior to the orbital septum. It then takes a more vertical course toward the Whitnall ligament (superior transverse ligament).
The Whitnall ligament is similar to the previously described orbital fascia and lies in close proximity to the aponeurotic and muscular junction of the LPS. It extends around the upper margin of the orbit in a plane that lies between the lacrimal gland fascia and the trochlea. The LPS varies in thickness, and is relatively thin in areas between the upper orbital rim and the Whitnall ligament.
When traced inwards and outwards, the LPS aponeurosis forms ‘horns’ called medial and lateral horns. The lateral horn runs through the lacrimal gland, dividing it into 2 lobes - the palpebral lobe and the orbital lobe. Having done this, it goes on to attach to the lateral retinaculum located at the lateral orbital tubercle. On the other hand, the medial horn has a more direct course and is fixed to the posterior lacrimal crest.
The aponeurosis eventually reaches the border of the superior tarsal plate having fused originally with the orbital septum. At the bottom end of this fusion, a small part of the aponeurosis attaches to the lower aspect of the anterior part of the tarsal plate. One part of this fusion extends forwards to insert into the pretarsal orbicularis oculi muscle and skin, resulting in the formation of the skin crease in the upper eyelid.
Fat Pads
There are a number of different fat pads that are present within and around the eyelid. One layer of fat called the pre-aponeurotic fat is found right behind the orbital septum and in front of the levator aponeurosis. Also within the upper eyelid are two more areas that contain fat pads that are centrally and medially (towards the nose) located. The medial fat pad is pale yellow in colour and lies in front of the levator aponeurosis.
On the other hand, the central pad of fat is broader and yellow in colour. As it travels outwards, it wraps around the inner aspect of the lacrimal gland. The lacrimal gland can be clearly seen and differentiated from this fat by its pink colour and lobulated structure. The lacrimal gland is positioned just posterior to the orbital margin but could prolapse slightly making it more prominent when the eye is examined.
While the above described the fat pads within the upper eyelid, the lower eyelid fat pads are slightly different in structure. The inferior oblique muscle separates the central fat pad from the dinner medial fat pad. There is a small amount of fat that lies in front of the inferior oblique muscle as well. The inferior oblique muscle originates from a small indentation in the lower border of the orbital floor, moving behind the orbital margin and at the upper aspect of the nasal lacrimal canal. It passes underneath the inferior rectus muscle and through the Tenon capsule, ultimately inserting at the point close to the macula of the eye. This rather winding course of the inferior oblique muscle makes it vulnerable to injury during this section of the fat pads around the eyelid and eye.
Blood supply
The eyelids are supplied by branches of the internal and external carotid arteries. The ophthalmic artery branches off the internal carotid artery and supplies different parts of the eyelid. At the inner part of the upper eyelid, the ophthalmic artery splits into two and traverses outwards the supply both the upper and the lower eyelid. The branch that supplies the lower eyelid is in fact a branch that arises from the superior marginal vessel (that supplies the upper eyelid). The superior and inferior marginal vessels that arise from the ophthalmic artery together form the marginal arcade.
The marginal arcade arteries are located at the front of the tarsus, 4 mm from the upper eyelid and 2 mm from the lower eyelid margin each. The superior marginal arcade gives rise to a peripheral arcade that runs in front of the Muller muscle, giving it a superficial plane and making it prone to injury during eyelid surgery. The peripheral arcade in the lower eyelid is often rudimentary.
Another branch of the internal carotid artery is the lacrimal artery that passes through the orbital septum along each eyelid and ultimately joins the marginal arcade.
While the above described the branches of the internal carotid artery, the external carotid artery supplies the eyelids as branches of the facial artery, infraorbital artery and the superficial temporal artery. Each of these pride branches that anastomosis with other arteries on the face. For example, the branch of the superficial temporal artery that supplies the eyelids joins with the zygomatic branch and transverse facial branch.
Lymphatic drainage
The lymphatic drainage of the eyelid is rather extensive. The majority of the upper eyelid and the outer half of the lower eyelid drain into the pre-auricular lymph nodes, while a small part of the middle of the upper eyelid and the inner half of the lower eyelid drains into the submandibular lymph nodes.
Muscles
There are numerous muscles around the eyeball that control of different movements. These muscles are called extraocular muscles. They include the medial rectus, lateral rectus, inferior and superior oblique and inferior and superior rectus muscles. These are responsible for the various directions of movement of the eyeball, including rotation of the eyeball. Within the eyelid, the levator palpebrae superioris is responsible for elevation of the upper eyelid.
The extraocular muscles are supplied by a variety of different cranial nerves. These include the oculomotor nerve, the trochlear nerve and abducens nerve.
Bones
The socket within which the eyeball is located is called the orbit. It is a pyramidal shaped fossa that is created by the fusion of different orbital bones. These bones originate from the different aspects of the skull such as the frontal bone, sphenoid bone, zygomatic bone and the Palatine bones. In adds to, the maxillary bone and the lacrimal bone also form a part of it. The arrangement of these bones is such that the walls are parallel to each other. The orbit measures 4 cm in height, 3.5 cm in width and is around 5 cm in depth.
Within the orbit are a number of blood vessels and nerves. These passed through the bone through various openings called fissures. There are three main openings - the superior orbital fissure, the inferior orbital fissure and the optic canal. Through these openings, various cranial nerves passed through and supply the muscles and blood vessels in the orbit. The superior orbital fissure allows for the passage of the frontal nerve, lacrimal nerve, nasociliary nerve and the recurrent branch of the lacrimal artery along with the superior orbital and ophthalmic veins. The inferior orbital fissure allows for the passage of the infraorbital nerve, zygomatic nerve, infraorbital artery and vein and parasympathetic nerve supplying the lacrimal gland. Through the optic canal passes the optic nerve, central retinal vein and ophthalmic artery.
Lacrimal gland
The lacrimal gland is responsible for tear production. It is divided by the levator aponeurosis into an orbital lobe and a palpebral lobe. It has a characteristic appearance as has been previously described. It is supplied by the lacrimal nerve which is a branch of the ophthalmic division of the trigeminal nerve.
The lacrimal gland secretes tears that are drained through a series of ducts. The lacrimal system consists of lacrimal papillae, canaliculi, lacrimal sac and naso-lacrimal duct. The canaliculus joins the lacrimal sac at an angle which is protected by the valve of Rosenmuller.
Connective tissue
We have already taken a brief look at the different types of connective tissue that are seen in the eyelid and the structures around it. The fascia that is present around the eyeball divides the orbit into a number of different connective tissue planes. Within each of these planes lie different structures. Having a knowledge of the structures helps the surgeon in locating them.


.jpg)

